 Last week I shared about my journey with acupuncture as a relief method for my chronic pregnancy pain. In the post, I mentioned that this week I’d be flipping the conversation about pain to something more specific, but still a topic that has a place in my medical history nonetheless. That is Rheumatoid Arthritis.
Last week I shared about my journey with acupuncture as a relief method for my chronic pregnancy pain. In the post, I mentioned that this week I’d be flipping the conversation about pain to something more specific, but still a topic that has a place in my medical history nonetheless. That is Rheumatoid Arthritis.
I have a very distinct memory of being in grade 5 and consistently complaining to my mom about joint pain. Because my dad had dealt with a lot of chronic pain that was never diagnosed, I think my mom was taking my pain very seriously and wanted to be proactive about it.
side note: my dad passed away when I was 9 which is why he was never diagnosed with arthritis. We now believe that he had ankylosing spondylitis (an arthritis of the spine) as his sister has since been diagnosed with it.
While I was never diagnosed with any form of arthritis at that time, I did end up doing a big project specifically on Rheumatoid Arthritis that I presented to my grade 5 class. I learned a lot about RA during that process and have actually been interested in the disease ever since. Flash forward 17 (give or take) years and pain is something that still affects not only me but also my husband.
My husband has thought for a long time that he may have some form of arthritis (he tested negative for the RA factor, but I’ve now learned this marker doesn’t necessarily mean you do/don’t have arthritis). Jamie deals with a lot of pain and swelling of his joints, and now after chatting with Dr. Baer, (more below) I really do think we should look further into his pain. When it comes to my pain, it is pregnancy-related. However, prior to becoming pregnant, chronic back pain was something I dealt with so I was tested for ankylosing spondylitis. Thankfully, those imaging test results are currently negative. Because of my pain, it has made me extremely empathetic to those who have an autoimmune disease like RA as it truly affects your quality of life.
When I look at these photos of my family and I playing, laughing, and having a good time at the beach, it makes me feel so grateful that we have our health and can do these things. However, I will say that in between these very carefree moments is a pregnant gal who is walking around in a lot of pain, and my husband, who despite his pain, will still throw our son up into the air and act like everything is a-ok! Our pain is clearly manageable on this day, but when someone is having an RA flare-up, it may not be possible to things like we’re doing here or even get out of bed. This is why I want to draw more awareness to this disease and what exactly it is.
I am not a doctor (surprise!) but I was lucky enough to get in touch with one! Rheumatologist, Dr. Phillip Baer, graciously took the time to have an over the phone conversation with me about Rheumatoid Arthritis. I personally learned so much about Rheumatoid Arthritis and found it all quite fascinating (did you know there are actually 150-200 types of arthritis but RA is the most common?). With that, I wanted to share our q&a below. As always, please let me know if you found this post interested or helpful and if you have any other questions, I’d be happy to find answers for you!
I’m also going to share The Talk Over RA website here as it is a great resource if you or someone you know suffers from Rheumatoid Arthritis. There are lots of facts and even a discussion guide to share with your doctor which can be very helpful during appointments.
 To begin, what exactly is arthritis. Are there different types and how is it diagnosed?
To begin, what exactly is arthritis. Are there different types and how is it diagnosed?
Arthritis simply means inflammation of the joints. Arthritis is often an autoimmune and inflammatory disease. There are actually 150-200 types of arthritis, but the most common inflammatory type in women is Rheumatoid Arthritis (RA). RA causes inflammation (painful swelling) because your immune system is mistakenly attacking healthy body tissue. Some signs of rheumatoid arthritis are soft tissue swelling and fluid in the joints. Joint pain and stiffness are typical symptoms, as is fatigue, We typically diagnose arthritis in a few ways. We take a history and ask questions to the patient about what is going on with them physically, we ask about certain features of their arthritis (i.e. is it a man or woman, what is their age, etc.), and then we do a physical exam and check if the joints are tender or swollen. For example, if we see a woman in her 40’s-50’s who has soft tissue inflammation in her finger knuckles and wrists, it is likely RA. There are also other blood tests like the Rheumatoid Factor test, CCP Antibody test, and blood tests for inflammation (ESR, CRP) and blood counts. Lastly, we can do imaging like x-ray, ultrasound, and sometimes MRI to help diagnose the patient.
 What are some causes of Rheumatoid Arthritis?
What are some causes of Rheumatoid Arthritis?
We don’t know the exact cause of RA but it’s certainly much more common in women than in men, which means there is a hormonal influence playing a factor. Genetics play a factor and genetic markers can be found through more sophisticated testing. Smoking cigarettes is also a risk of getting RA. Research studies show that certain bacteria in the lungs and mouth can be linked to a higher risk of developing rheumatoid arthritis.
 What are some things I can do at home to alleviate the pain?
What are some things I can do at home to alleviate the pain?
-Resting and pacing activities if you are having an inflammation flare-up.
-Exercise is good for you in between flare-ups because it protects and preserves your muscles, ligaments, and tendons around the joints.
-Heat/ice, hot bath/shower, hot pack can be soothing for more chronic RA pain.
-Meditation or anything that can help you sleep better and relax.
-Over the counter medication such as Tylenol, ibuprofen, naproxen, and topical anti-inflammatory rubs.
 What are the other treatment options available? I’d love to hear both from a doctors perspective (medication wise) & if you know of any remedies like acupuncture, etc.
What are the other treatment options available? I’d love to hear both from a doctors perspective (medication wise) & if you know of any remedies like acupuncture, etc.
Natural Remedies:
-Acupuncture: people do use acupuncture as a treatment but there isn’t enough evidence to support that it works for RA.
-Physiotherapy and massage can make you feel better and lessen symptoms.
Medications:
Medications depend on the type of arthritis. For RA, the basic treatment would be anti-inflammatory medication which are the prescription versions of ibuprofen, naproxen and diclofenac. A more advanced treatment would be Disease-modifying drugs (DMARDs) which, for example, are drugs such as Hydroxychloroquine and methotrexate. Hydroxychloroquine is a relatively safe and well-tolerated drug for the treatment of mild rheumatoid arthritis. We also may use steroid joint injections to help treat Rheumatoid Arthritis. The injections are very safe, but steroid tablets have a lot of side effects and are reserved for short-term use or more severe symptoms.
There are also new drugs that have come out within the last 20 years which are called biologics. They are given by injections or IV infusions. Oral advanced therapies called JAK inhibitors have been around for about 7 years and perform as well as biologics do, but are taken orally once a day.
 Can my diet affect my pain? Are there certain foods that help with inflammation? What about supplements?
Can my diet affect my pain? Are there certain foods that help with inflammation? What about supplements?
An anti-inflammatory diet may help you; foods such as fish, fruits and veggies are all good to take if you have RA but there isn’t concrete evidence to support it will make a huge difference. Turmeric (curcumin) may help to reduce inflammation as well and there are some studies that show it can help. With arthritis such as gout, diet plays a big role as it can be triggered by red meat, seafood, sugary pop, alcohol, etc.
Supplement wise, Omega 3’s, Glucosamine, chondroitin, and vitamin D may help in some patients to alleviate some symptoms.
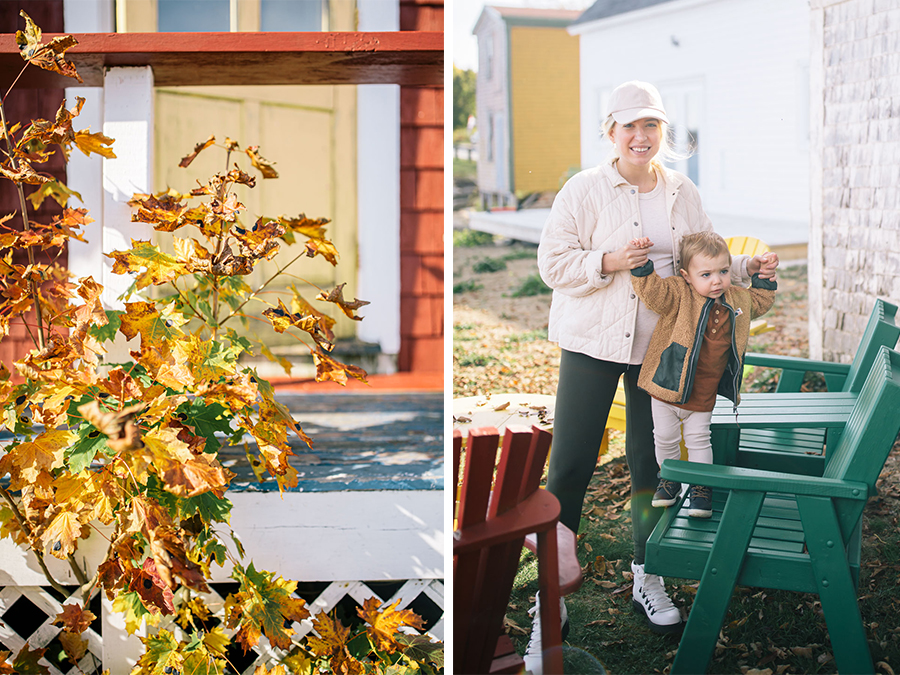 Who is most likely to be diagnosed with RA?
Who is most likely to be diagnosed with RA?
Women by 3 to 1. We actually used to find that a woman who had recently given birth was more susceptible to RA because of hormonal changes (which does happen). Today, we have found that women in their 40’s-50’s are at the most common age to be diagnosed.
 Can exercise help my RA or make it worse? What types of exercises should I be doing?
Can exercise help my RA or make it worse? What types of exercises should I be doing?
Yes, but not if you are having an acute flare-up as mentioned. Exercise otherwise is great to help preserve your range of motion, strengthen your muscles, and maintain the flexibility of the tendons and ligaments that help support your joints. Types of exercises that are good for someone with RA are low impact. Things such as light aerobics, walking, swimming, stretching, core strengthening, pilates, yoga, tai chi, etc. are all great options.
 Is RA hereditary?
Is RA hereditary?
It can run in families because of the genetic predisposition. But I would say that most of the patients I have with RA are the only ones in their family to have the disease. If you have RA, I wouldn’t spend a lot of time worrying that your children may get the disease, as the genetic component isn’t the biggest thing
 This post was brought to you by Talk Over RA
This post was brought to you by Talk Over RA



